Food and food choices may be a touchy subject for your loved one. Food choices are one of the few things over which a cancer patient has control. At times, your loved one may be resistant to eating. Try to encourage your loved one to eat but don’t be too forceful. Cancer treatment is an emotionally challenging time. Don’t let disagreements over food turn into full-blown fights or arguments. Reach out to the healthcare team for support and resources.
Influences on Food Choices
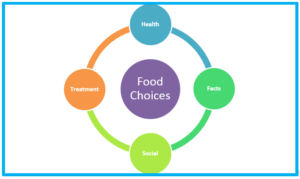
As you look at this diagram, you can see that many factors influence a cancer patient’s food choices—health, treatment, facts, and social factors. For example, a patient may know the fact that food promotes healing, but if the patient feels nauseated after chemo treatment, he or she may not want to eat. Even if a patient’s health isn’t strong enough for alcohol, he or she may feel social pressure to drink when out with friends. These are just a few examples of how these factors may interact.
Food provides valuable nutrients for cancer patients. Eating well during cancer treatment can help speed recovery, ease side effects, and keep the treatment plan running smoothly. However, your loved one may not be able to plan grocery lists, grocery shop, eat, digest foods, or prepare meals like before cancer. This is where you as the caregiver can help. Depending on the health of the patient, you may need to assist with
- Grocery shopping
- Meal prep and cooking
- Encouraging the patient to make healthy food choices
- Managing the patient’s treatment side effects.
As a caregiver, there are many ways you can assist with food and meals. To get started, ask the healthcare team about specific foods or meal recommendations and restrictions, if any. A printed meal plan or food list is best. Ask to speak to a registered dietitian for help.
During cancer treatment, there may be times when your loved one needs to follow a special diet. Some examples of special diets include: clear liquid, full liquid, low-fiber, or low-iodine. The first three diets listed are common after surgeries that affect the digestive system. If the patient has thyroid cancer, he or she may need to be on a low-iodine diet while receiving radioactive iodine treatment. The healthcare team will let you know when a special diet is needed and provide you with specific guidelines to follow. Ask to speak to a registered dietitian for extra help. Visit Sample Menus to see examples of menus for specific needs. Use the Meal Planning Worksheet to plan a week’s worth of meals.
Foods that you or a healthy person can eat may not be what a person with cancer can eat. Even what one cancer patient can eat may be different from what another cancer patient can eat. You and the patient may be bombarded with stories of “miracle” foods and diet tips by well-meaning family and friends. Remember—if something is too good to be true, it probably is. Always consult the healthcare team to know what’s best for your loved one.
Food choices are one of the few things over which a cancer patient has control. In some cases, food and food choices may be a touchy subject for your loved one. The patient may be resistant to eat at times. Try to encourage the patient without being too forceful. Cancer treatment is an emotionally challenging time. Before disagreements over food turn into full-blown fights or arguments, turn to the members of the healthcare team, counselors, spiritual advisors, or other resources to help sort out any differences that may arise as you attempt to care for your loved one.
Schedule a consultation with PearlPoint’s registered dietitian to learn more about caring for your loved one during cancer treatment.

